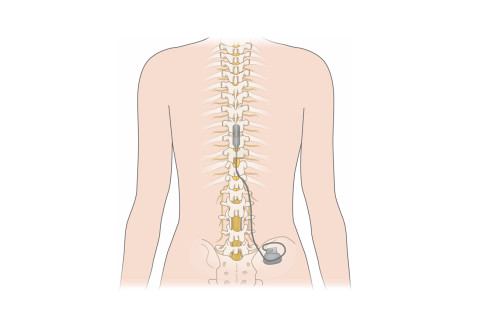
Spinal cord stimulation is an effective and safe treatment for persistent lower extremity radicular nerve pain after spinal surgery, according to the doctoral thesis of Mette Nissen, MD. Notwithstanding, proper patient selection is essential for a successful outcome.
The purpose of Nissen’s doctoral thesis was to study long-term outcome of spinal cord stimulation in the treatment of severe and long-lasting radiating neural root pain after lumbar surgery. In spinal cord stimulation mild electric currents are applied to the spinal cord through small medical devices, altering pain processing in the central nervous system and replacing pain sensation with mild paraesthesia.
Long-term outcomes were defined as adherence to the spinal cord stimulation treatment throughout the follow-up and capability to discontinue strong opioids or significantly reduce their use. Patient satisfaction was measured through a postal questionnaire at the end of follow-up. The safety of treatment was measured as the number of adverse effects. Concomitant use of gabapentinoids and other neuropathic medication and their effect on spinal cord stimulation outcome was assessed. Study cohort included all 224 consecutive patients trialled for spinal cord stimulation at the Kuopio University Hospital from 1996 to 2014. The median follow-up time was six years.
After one-week trial, permanent spinal cord stimulator was implanted in 78 percent of patients. During the median follow-up of six years, 19 percent of patients had their device explanted due to inadequate pain relief, and six percent for other reasons. One hundred and thirty patients continued with spinal cord stimulation until the end of follow-up. Of these, 47 percent returned the questionnaire, and 69 percent reported substantially improved or better outcomes. Electrode revision due to inadequate pain relief was done for 22 patients.
Risk of treatment failure was highest in patients with high-dose opioid use; daily use of 35 morphine milligram equivalents was the optimal cut-point value. One patient out of four who continued to use spinal cord stimulation throughout the follow-up was able to discontinue all opioids, but none of the patients who had their device explanted or revised due to insufficient pain relief.
Gabapentinoid users had significantly lower risk of stimulator explantation and were significantly more often able to reduce their opioid dose by more than 50 percent. Gabapentinoid benefits as adjunctive therapy to spinal cord stimulation should be verified in a randomized controlled trial.
The doctoral dissertation of Mette Nissen, Licentiate of Medicine, entitled Long-term outcome of spinal cord stimulation in failed back surgery syndrome, will be examined at the Faculty of Health Sciences. The Opponent in the public examination will be Professor Maarten Moens of University Hospital Brussels, and the Custos will be Docent Mikael von und zu Fraunberg of the University of Eastern Finland. The public examination will be held in English.