Knee joint injuries, such as anterior cruciate ligament (ACL) rupture, are common in athletes. As the intact joint ligaments offer a precondition for joint stability, the ACL ruptures are often surgically reconstructed. However, in many cases, ACL injury or surgical reconstruction has shown to lead to post-traumatic osteoarthritis (OA). OA is the most common musculoskeletal joint disease, in which primarily the articular cartilage and subchondral bone are degenerated causing unbearable pain within a joint. OA affects more than 250 million people and places a huge financial burden on both the patient and the society.
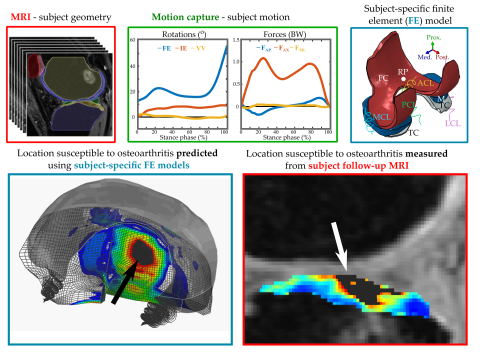
Preventing the onset and development of osteoarthritis would be cost-effective and helpful. However, prevention is possible only if the disease development can be predicted. Computational modelling can be used to predict locations susceptible to osteoarthritis. To create patient-specific models, three inputs are required: geometry, motion and material property. While the knee geometry can be obtained from clinical magnetic resonance imaging (MRI) and motion can be measured via utilization of reflective skin markers, an accurate information from failure properties of soft tissues remains unknown. Thus, the greatest limitation of these computational models is the lack of result verification.
In this thesis, a fast and reliable method of implementing patient-specific motion into computational models was developed. Using this method, patients with ACL reconstruction at risk of developing knee joint OA were identified. Different degenerative mechanisms, such as excessive cartilage deformations and stresses, were assessed. To verify the computational model reliability, the model predictions were compared against structural and compositional changes assessed using advanced MRI techniques.
The findings of this thesis revealed that simplified and faster models yield similar results as more complex and computationally intensive models. Additionally, these locations susceptible to OA onset and progression predicted by these simplified models matched clinical follow-up information. Therefore, the presented computational approach could be utilized to identify patients at risk of developing OA in a clinical setting and could reveal optimal and personalized rehabilitation and prevention protocols to prevent or delay the disease progression.
This study has received funding from the University of Eastern Finland’s doctoral programme in science, technology and computing (SCITECO), Academy of Finland, Sigrid Juselius and Orion Research Foundations.
The doctoral dissertation of MSc Paul Octavian Bolcos, entitled Finite element modeling of anterior cruciate ligament reconstructed knee joints: toward clinical use via fast motion implementation and verification against MRI follow-up, will be examined at the Faculty of Science and Forestry on the 19th of February at 3 PM online. The opponent of the public examination will be Professor Amy Lerner, University of Rochester, USA, and the custos will be Professor Rami K. Korhonen, University of Eastern Finland. The public examination will be held in English.