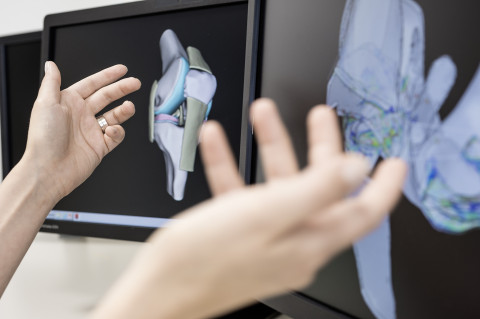
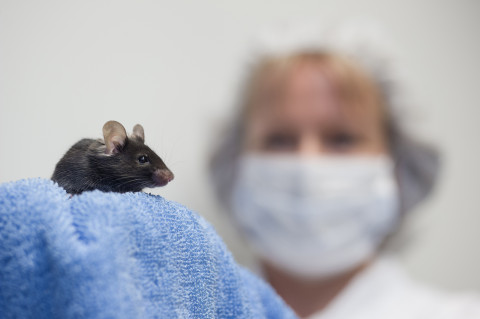
The A.I. Virtanen Institute for Molecular Sciences is a research institute that responds to the global health challenges created by the aging of the population and changes in lifestyle by focusing on the research of cardiovascular and brain diseases. The A.I. Virtanen Institute for Molecular Sciences maintains and uses several parts of the core university infrastructure, such as the Kuopio Biomedical Imaging Unit, the National Virus Vector Laboratory as well as the Lab Animal Centre.
The institute participates in postgraduate education in the Doctoral Programme in Molecular Medicine, and it also participates in the teaching of the Master’s Degree Programme in Biomedicine.
Research
The research of the A.I. Virtanen Institute for Molecular Sciences is based on the Ageing, Lifestyles and Health profile area in the university’s strategy. The institute’s key research areas include cardiovascular diseases, brain diseases and cancer. The institute’s field of research is molecular medicine, which studies the causes and mechanisms of diseases on the molecular and cellular levels and applies the information to the prevention, diagnostics and treatment of diseases. The research takes advantage of cell and animal models as well as advanced in vitro and in vivo imaging technologies.
Our research groups are a part of the university’s strategically significant Research Communities (RCs): Neuroscience, Metabolic Diseases, Basic, Translational and Clinical Cardiovascular Medicine, and Multidisciplinary Cancer Research.
Neuroscience
- Baran Aydogan group: Computational Neuroimaging Group
- Olli Gröhn group: Biomedical MRI
- Annakaisa Haapasalo group: Molecular Neurodegeneration
- Katja Kanninen group: Neurobiology of Disease
- Sarka Lehtonen group: Human Brain Disease Modelling
- Tarja Malm group: Neuroinflammation Research
- Riikka Martikainen group: Stem cells and mitochondria
- Asla Pitkänen group: Epilepsy Research
- Alejandra Sierra Lopez group: Multiscale Imaging Group
- Heikki Tanila group: Neurobiology of Memory
- Jussi Tohka group: Biomedical Image Analysis
Metabolic Diseases
- Minna Kaikkonen-Määttä group: Cardiovascular Genomics
- Pasi Tavi group: Molecular Physiology
Basic, Translational and Clinical Cardiovascular Medicine
- Minna Kaikkonen-Määttä group: Cardiovascular Genomics
- Mikko Kettunen group: Metabolic MR Imaging Group
- Johanna Laakkonen group: Vascular Biology
- Nihay Laham Karam group: Translational Vectorology
- Seppo Ylä-Herttuala group: Molecular Medicine
Multidisciplinary Cancer Research
- Anna-Liisa Levonen group: Redox Signaling
Our research environments
Let’s talk science.
Heikki Tanila
Professor, Head of the A.I. Virtanen Institute for Molecular Sciences

Studies
The A.I. Virtanen Institute for Molecular Sciences participates in postgraduate education in the Doctoral Programme in Molecular Medicine, and it also participates in the teaching of the Master’s Degree Programme in Biomedicine. The basic education courses arranged by the institute include courses at the Lab Animal Centre. The institute also arranges international doctoral courses annually and offers individual courses for exchange students and international trainees.
News and events
News
Events
Social media
Contact information
General administration
Joanna Huttunen
Personnel administration
Tarja Salmi and Sanna Partanen
Laboratory equipment and maintenance
Jari Nissinen
Financial affairs
Taisto Kuosmanen
Get acquainted with our personnel in UEF Connect search service.
Postal address
University of Eastern Finland
A.I. Virtanen Institute for Molecular Sciences
P.O. Box 1627
FI-70211 KUOPIO
FINLAND
Street address
Neulaniementie 2
Bioteknia building